At the heart of saving lives
The Peter Munk Cardiac Centre has helped transform survival rates for people with failing hearts. Here’s how it developed one of the world’s largest and most successful heart failure programs
When Sravan Vemuri was in his third year of medical school in spring of 2019, he practiced doing an electrocardiogram (ECG) on himself during a cardiac clinic rotation. The 26 year old put electrodes on his chest and noticed his results were oddly similar to those of a patient with longstanding heart disease. An attending physician checked the machine and ran the test again. “I was trembling,” recalls Vemuri of waiting through that second test.
The same results came back. The physician took him aside. “I’m really sorry, but you’re somehow in heart failure,” he told the normally athletic student.
Shocked but determined to finish medical school, Vemuri struggled with his worsening health. He was referred to the Peter Munk Cardiac Centre where he received a pacemaker and was put on medications after his first appointment. But by fall 2021, his heart failure had progressed significantly; shortness of breath made it difficult for him to walk more than a few steps.

Dr. Adriana Luk, advanced heart failure and transplant cardiologist and Head of the Coronary Intensive Care Unit at the Peter Munk Cardiac Centre, told Vemuri his medications were no longer effective in addressing his progressing heart failure, and he needed a heart transplant.
We offer best care and team care for the most complicated patients.
Dr. Michael McDonald
While waiting for a donor heart his doctors effectively managed his condition and offered him the latest VAD – a ventricular assist device to help keep his heart pumping – but it was challenging for Vemuri to stay optimistic. He credits his nurse practitioners and nurses for extending their compassion and giving him hope and says he received care from every corner of the Peter Munk Cardiac Centre, including custodian Jared Wright, who visited him each morning and became an important figure in his life.
In February 2022, a match became available and the team at the Peter Munk Cardiac Centre and University Health Network’s (UHN’s) Ajmera Transplant Centre performed heart transplant surgery.
The care Vemuri received from this world-class team has been built on a legacy of innovation.
“We have raised the bar to a higher level,” says Dr. Tirone David, world-renowned cardiac surgeon at the Peter Munk Cardiac Centre and UHN’s Sprott Department of Surgery, who has been part of that history. Better medications and improved procedures – some developed at the Peter Munk Cardiac Centre – now allow people to live longer than ever with heart disease.
“We have raised the bar to a higher level.”
Dr. Tirone David
And although surgical advancements and new therapies are available to treat the growing number of people with heart disease, there are still patients where heart transplant is their only option. As the number of available organs remains flat, the Peter Munk Cardiac Centre team continues to perform up to 42 heart transplants per year – the most in Canada – while pioneering surgical techniques and keeping people with heart failure off the transplant list.
Decades of fine-tuning innovations
When Dr. David, who also holds the Melanie Munk Chair in Cardiovascular Surgery, joined what is now UHN about 40 years ago, the heart transplant program did not exist. He fostered numerous improvements in surgical procedures to treat heart disease, including developing various operative procedures and heart valve substitutes now used globally. But with patients still experiencing end stage heart failure and requiring transplants, Dr. David founded the heart transplant program at the Peter Munk Cardiac Centre. He then began building an ecosystem of innovation around transplantation and helping heart failure patients live longer. These changes were supported by the introduction of effective anti-rejection drugs that helped people being treated with end-stage heart disease live better after transplant.
By the early 2000s, doctors had access to better medications specific for heart failure; they could give patients ace inhibitors and beta blockers to help heart muscle stay strong while waiting for transplant. “The name of the game was to get people on the right drugs and keep them out of hospital and try to change their prognosis,” says Dr. Michael McDonald, Medical Director of the Advanced Heart Failure and Heart Transplant Program at the Peter Munk Cardiac Centre and UHN’s Ajmera Transplant Centre.
“The original focus of the Peter Munk Cardiac Centre’s Heart Function Clinic was to do advanced prognostication. That’s probably one of our defining features.”
Dr. Michael McDonald
Now, the development of new drugs, better surgical techniques and mechanical heart implants act as a bridge for patients at the Peter Munk Cardiac Centre awaiting a donor heart. Dr. David notes, “These developments along with having a team of dedicated experts allow us to treat those who would not have been heart transplant candidates when the program started.”
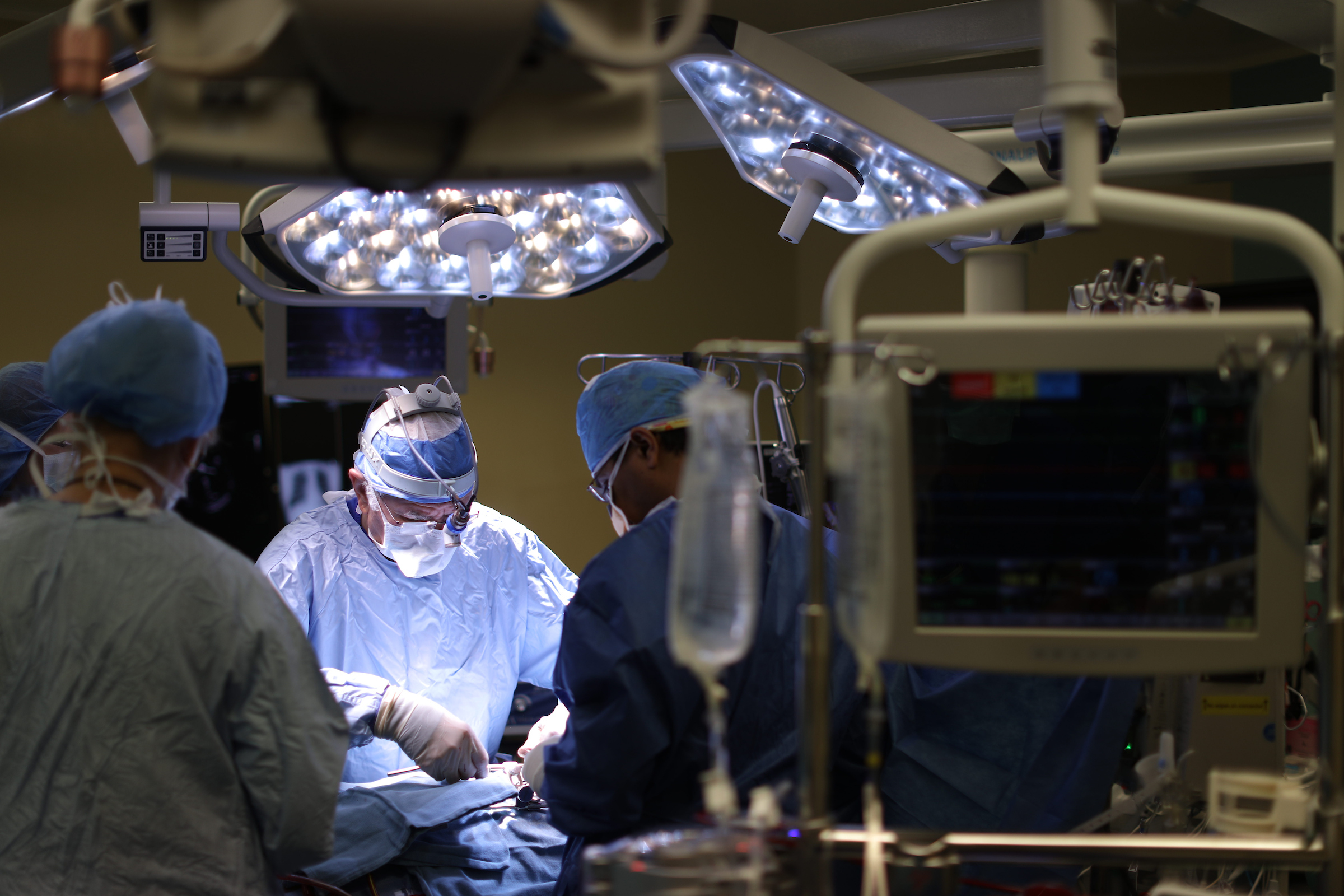
Specialized and next level approaches
The heart failure and transplant teams specialize in understanding which patients will respond well to which treatment. “The original focus of the Peter Munk Cardiac Centre’s Heart Function Clinic was to do advanced prognostication,” says Dr. McDonald. “That’s probably one of our defining features.” This expertise has helped the team choose wisely from the ever-growing treatment options available, and create truly personalized medicine.
21%
Patients at the Peter Munk Cardiac Centre have a 21 per cent lower risk of developing coronary artery disease in a transplanted heart at 10 years post-transplant and a 15 per cent lower risk of developing rejection, in which the recipient’s immune system “rejects” the donor heart.
To advance the assessment of which factors impact heart outcomes, the Peter Munk Cardiac Centre helped develop and host a national cardiac transplant and implanted device database. “All Canadian transplant programs will be able to share data and evaluate how we are improving outcomes,” says Dr. McDonald, who believes the two-year-old, beta level database will be a boon for researchers once developed.
Meanwhile, technology now exists to support hearts outside the body for many hours before transplantation in a special organ care system. “The heart can travel greater distances, and you can keep the heart beating and assess its function,” says Dr. McDonald, who says the team is about to obtain one of these machines, which have been proven to increase the number of donor hearts suitable for transplant.
Further, current research at the Peter Munk Cardiac Centre involves creating an Ex Vivo Organ Perfusion System for the heart – pioneered by UHN in 2008 for lungs. This innovative therapy applied to a donor heart outside of the body before transplantation improves the organ quality and can make hearts that were previously unsuitable for transplant safe to use.
Dr. David reveals, “In the future, this technology could even change the immunological response when a heart is implanted in the recipient, minimizing the risk of rejection.”
Optimizing care in a huge network
Since Dr. McDonald joined the Peter Munk Cardiac Centre team in the late 2000s, it has grown dramatically in both size and discipline. “People realized this is a team sport,” he explains. “You build a huge network to support patients upfront and offer optimal care as quickly as possible.” Now with 10 heart transplant cardiologists and a sizable nursing team, doctors with a range of expertise along with specialized pharmacists, dietitians and social workers are regularly involved.
“We have the depth and breadth to take care of any type of patient with heart disease,” explains Dr. David.
“Just a few decades ago, someone diagnosed with heart failure had a one-year mortality rate of 20 per cent. That’s down to about five per cent at the Peter Munk Cardiac Centre now,” says Dr. McDonald. “We’re offering dramatically better outcomes to patients living with heart failure compared to 15 years ago, even compared to five years ago.”
“That is my goal. I will get there.”
Sravan Vemuri, on completing a medical residency in cardiology
That includes Vemuri, whose heart transplant at just age 28, means he has a long life ahead of him, taking anti-rejection medications and having his health monitored by the team at Peter Munk Cardiac Centre.
To this day, Vemuri cannot forget the moment he was told by his doctor the good news of an available heart. Inspired by the tenacity and aptitude of the cardiologists at the Peter Munk Cardiac Centre, Vemuri says he is driven to develop a character as such.
Within weeks of surgery, Vemuri was home, signing up for recreational badminton and resuming his career plans, which include getting enough strength to do a medical residency, ideally in cardiology. Vemuri insists, “That is my goal. I will get there.”

